By Wesley Smith, Ph.D., HealthSnap Co-Founder & Chief Scientific Officer
Obesity is a pervasive and complex health concern affecting millions of people worldwide. It results from excess energy storage, and while lifestyle plays a critical role in the prevention and treatment of obesity, the condition often involves dysregulation of a fat mass setpoint. This means that contributing factors may occur subconsciously rather than volitionally.
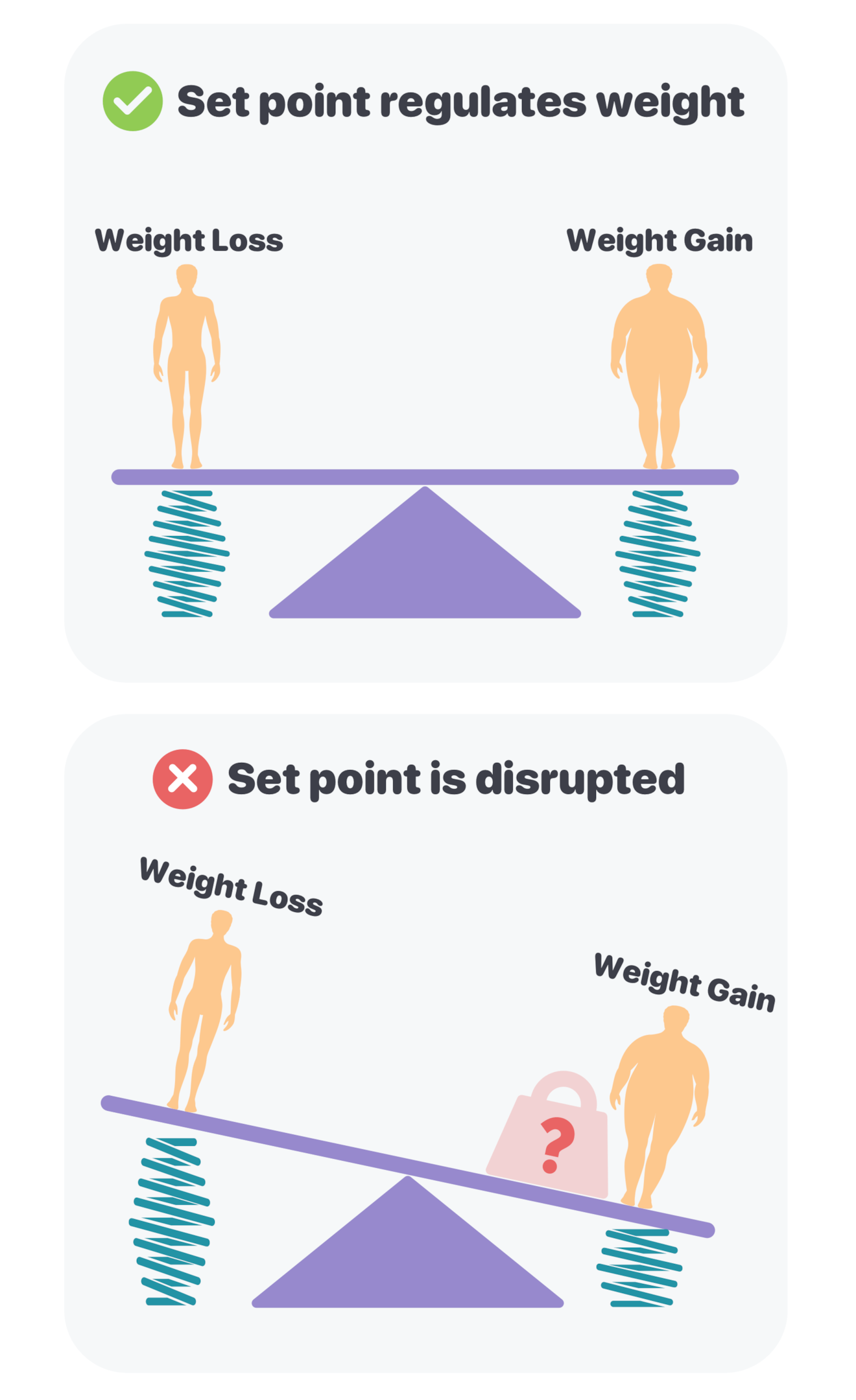
The aspects that contribute to excess weight and lipid accumulation in the body are diverse and intricate, encompassing neuroendocrine, metabolic, environmental, and psychological influences. Consequently, individuals may not be fully aware of the underlying reasons for their weight gain. If left unaddressed, obesity can lead to a myriad of chronic conditions and other risk factors such as diabetes, heart disease, and cancer. This formidable health challenge necessitates a comprehensive approach led by clinicians, utilizing all available innovative and modern methods.
Obesity and Psychological Effects
In addition to the well-known physical consequences of obesity, it is crucial for healthcare professionals to recognize the significant psychological effects that may accompany this condition. Obesity can lead to various mental health issues for adults, such as depression, anxiety, low self-esteem, and social isolation.
These psychological factors can further exacerbate the challenges faced by individuals struggling with obesity, creating a vicious cycle that may hinder weight loss efforts and overall well-being. To help break this cycle and guide patients on their journey toward better health, regular consultations with a healthcare professional are essential.
These consultations can provide personalized support, monitor progress, and keep patients on track, ensuring healthcare professionals take a holistic approach to healthy eating to address both the physical and psychological aspects of obesity in adults.
Obesity and Prescription Medicines in 2023
Addressing obesity and weight management in adults with prescription medicine has been historically challenging due to insufficient long-term efficacy and complexities in evaluating cardiovascular safety. However, Clinical trials with more recent prescription medicine, such as incretin-based therapies like Ozempic and Trulicity (GLP-1 agonists & DPP4-inhibitors), and SGLT-2 inhibitors like Jardiance, have shown promise.
These medicines work through different mechanisms: incretin-based therapies enhance the effects of incretin hormones such as glucagon-like peptide-1 (GLP-1) and blood sugar-dependent insulinotropic polypeptide (GIP) to stimulate insulin secretion and suppress glucagon secretion in a blood sugar-dependent manner, while SGLT-2 inhibitors lower blood sugar levels by inhibiting the sodium-glucose co-transporter-2 (SGLT2) protein in the kidneys, reducing blood sugar reabsorption and promoting its excretion through urine.
It is not surprising that medicine for glycemic control shows potential in fighting obesity, given that insulin resistance often contributes to the obesity epidemic, as well as other health problems. Insulin resistance and the resulting hyperinsulinemia promote fatty acid synthesis and storage while inhibiting fat oxidation. A sedentary lifestyle combined with a diet rich in processed carbohydrates forms a hazardous blend that can overburden muscle glycogen stores. When there is insufficient capacity for glycogen storage, insulin resistance arises, as muscles are the primary location for glucose disposal. This underscores the value of a low-glycemic, whole-food diet and consistent exercise as strategies to enhance insulin sensitivity. The synergistic effect of these factors aids in reducing glycogen stores, which consequently improves glucose disposal, counteracts hyperinsulinemia, and fosters optimal metabolic function.
More than the Pill: The Power of RPM, CCM, and Pharmacotherapy
In light of this, recent obesity-treating trends focus on combining advanced pharmacotherapy with holistic lifestyle changes, such as a focus on nutrient-rich diets, exercise routines, stress management, and better sleep. However, what’s often missing in these approaches is the integration of modern technology and innovative remote care methods that make the process more engaging and effective for patients.
In fact, remote care management and monitoring can play an essential role in ensuring patient commitment and success, leading to healthier body composition and overall well-being. By harnessing the power of technology, we can create personalized, interactive experiences that keep patients motivated and committed to their health goals, emphasizing the importance of a comprehensive approach to treating obesity that includes both pharmacological interventions and behavioral modifications.
Takeaways:
-
Obesity is a complex, multifaceted global health issue with both physical and psychological effects.
-
Recent advances in pharmaceutical interventions, such as incretin-based therapies and SGLT-2 inhibitors, like Ozempic, taking Trulicity, and Jardiance, have shown promising weight loss results.
-
Combining pharmaceutical treatment with lifestyle changes, like diet and exercise, has become a popular trend in obesity management, but advanced technology and remote care methods can further enhance the effectiveness of these programs.
-
Insulin resistance is a major cause of obesity and is driven by inactivity and a highly processed carbohydrate diet.
-
Treating obesity requires a comprehensive approach, including both pharmacological interventions and lifestyle modifications.
-
A whole-food diet and physical activity have proven effective in reversing insulin resistance, hyperinsulinemia, and set point dysfunction to help with long-term weight management.
-
Integrating modern technology into obesity management strategies can create more engaging and personalized experiences to keep patients motivated and help them achieve their health goals.

Remote Patient Monitoring (RPM) & Chronic Care Management (CCM) for Obesity Management
Remote care management is critical to alleviating the limited bandwidth available to healthcare providers, enabling them more resources to delve into evidence-based lifestyle changes that can significantly complement treatment. Despite exercise being a highly effective intervention for patients with metabolic disease at risk of developing diabetes, there is a striking deficiency in its prescription among healthcare providers – a situation that, if pertaining to the prescription of a drug with comparable efficacy, could be perceived as negligence.
This highlights the need for better communication between healthcare professionals and patients regarding the importance of physical activity in managing metabolic disease, as well as the potential necessity for additional training and resources for physicians and healthcare providers to effectively promote exercise among their patients.
Bridging this gap in communication and education, remote care management emerges as a promising solution to address these challenges and optimize patient care, especially in the realm of obesity management. By utilizing trained Care Navigators to assist patients outside the practice through regular consultations and weight monitoring using an FDA-recognized cellular medical device, healthcare providers can gather information on the effectiveness of pharmacological treatments while also offering necessary guidance to develop effective lifestyle strategies to lose weight. This support helps keep patients motivated, with a lowered health risk, and on track toward their body weight goals. Additionally, healthcare providers can bill for RPM and CCM CPT Codes.
A study published in BMC Geriatrics demonstrated the positive impact of remote monitoring and care coordination on obesity management among older adults, incorporating regular phone consultations with healthcare professionals and a digital platform for tracking weight, appetite, and physical activity. Participants were able to lose weight, improve quality of life, and improved self-efficacy, indicating that remote care management can be both an effective and acceptable strategy for managing obesity and overall risk in this population.
Additionally, digital health programs often prove more cost-effective than traditional face-to-face care, resulting in savings for patients and healthcare systems alike. These programs also offer increased accessibility and convenience for patients who may face mobility or transportation challenges or reside in remote areas.
Consequently, hospitals and healthcare professionals should strongly consider advocating for the use of remote monitoring and care coordination when treating patients with obesity and other chronic conditions, like diabetes and heart conditions.
Takeaways:
-
Remote Patient Monitoring and care management are two key components of digital health programs that increase adherence to treatment plans, leading to better health outcomes and decreased health risk.
-
Remote care management has the potential to alleviate the limited bandwidth available to providers and help them to promote lifestyle strategies among their patients.
-
Remote monitoring and care coordination can help achieve weight loss, improved quality of life, and self-efficacy in managing obesity among older adults.
-
Digital health programs are cost-effective compared to traditional face-to-face care, making them more accessible and convenient for patients.
-
Healthcare professionals should consider using remote monitoring and care management when treating patients with obesity or other chronic conditions like diabetes, heart failure, and hypertension.
Digital Healthcare & Clinical Synergy
Remote monitoring provides significant benefits for patients using weight loss medications like SGLT-2 inhibitors and incretin-based therapies. These benefits encompass the ability to track body weight changes remotely, assisting in evaluating the patient’s response to treatment.
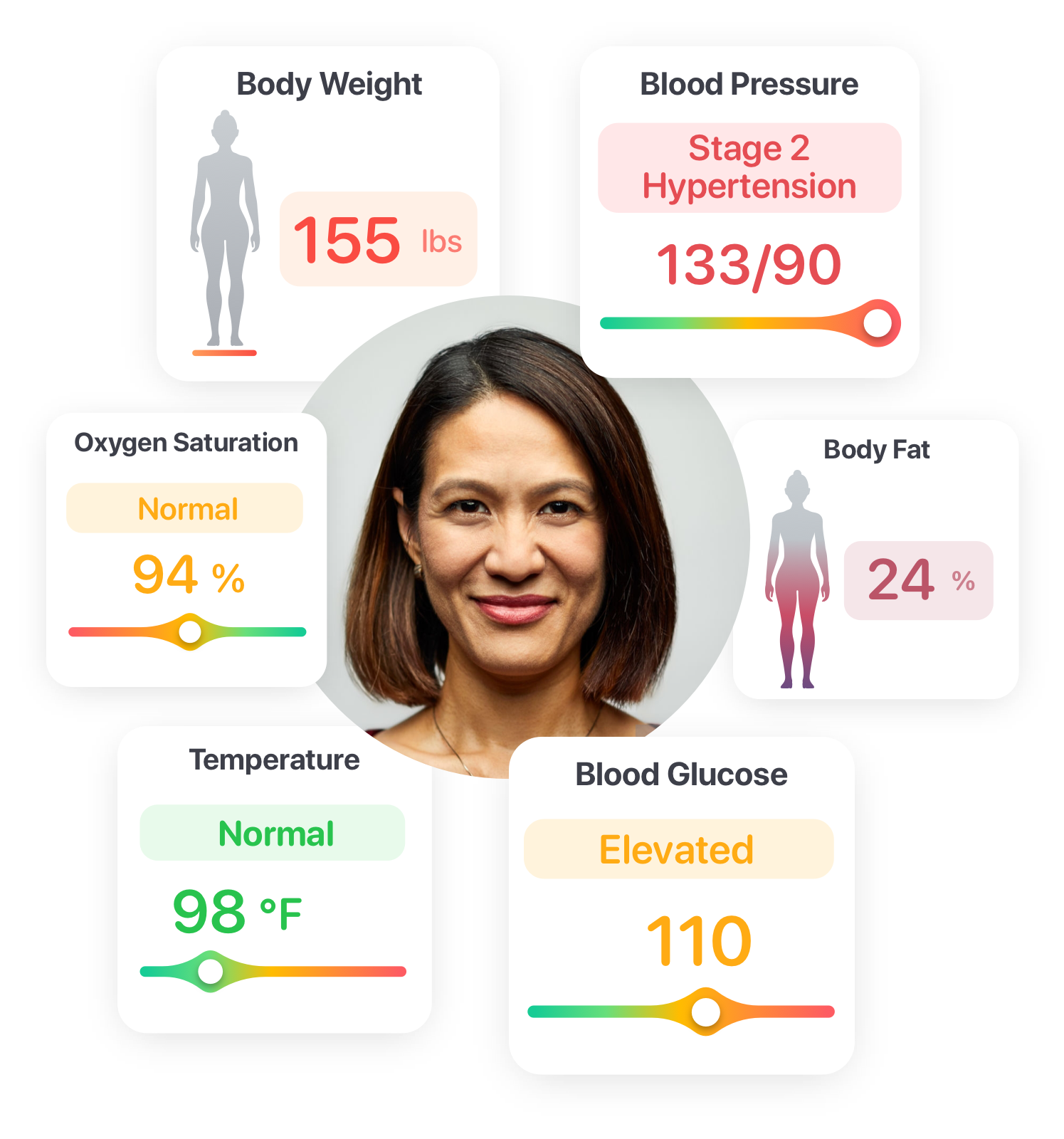
Additionally, remote monitoring with an RPM-approved medical device and other devices observes trends in blood pressure, blood sugar levels, and other vital health metrics, assisting in the identification of early warning signs of adverse events. This enables timely intervention to prevent hospitalization or additional complications.
To further enhance the effectiveness of obesity treatments, it is essential to adopt a holistic approach that incorporates complementary strategies such as diet and exercise for achieving a healthy weight and maintaining long-term weight loss. However, patients often face challenges in adhering to these lifestyle changes due to various barriers like lack of motivation, social support, and access to resources.
Remote Patient Monitoring and Personalized Weight Loss
Remote Patient Monitoring can help overcome these obstacles by offering personalized care navigation and education. For instance, remote consultations with a healthcare provider can assist patients in setting realistic goals, tracking their progress, and receiving feedback.
Additionally, remote monitoring tools, such as wearable activity trackers and cellular-enabled scales, can provide real-time feedback on physical activity levels, body weight changes, and heart rate, and motivate patients to stay engaged while tracking what they eat.

Comprehensive care for obesity must address multiple contributing factors, including stress management and sleep hygiene. Remote consultations can offer guidance on implementing stress-reduction techniques like mindfulness meditation, deep breathing exercises, mindful eating, and yoga, which contribute to overall well-being and healthier weight management. Care Navigators can also educate patients on the importance of sleep quality and quantity, providing strategies to improve sleep hygiene and maintain hormonal balance. By addressing these interconnected aspects and symptoms of obesity, remote care management empowers patients to make lasting lifestyle changes and achieve sustainable weight loss.
Takeaways:
-
Remote Patient Monitoring offers numerous advantages for patients taking recent medications to support weight loss and other conditions, including tracking changes in body weight, and blood levels to identify potential adverse events.
-
A complementary approach involving diet and exercise is essential for achieving long-term results; however, patients often face difficulties in adhering to lifestyle changes due to various barriers.
-
Remote care management can help address these challenges by providing personalized care navigation and education via telehealth sessions.
-
Real-time feedback from remote and specialized monitors, such as wearable activity trackers and cellular-enabled scales, can also encourage patients to stay motivated.
-
Counseling on multiple factors linked to obesity, including stress management and sleep hygiene, is vital for comprehensive care. Telehealth sessions can offer guidance on implementing stress-reduction techniques that contribute to overall well-being and healthier weight management.
Multidisciplinary Approach to Obesity Management and Weight Loss
Achieving successful weight loss necessitates a multidisciplinary approach involving healthcare providers, patients, and caregivers. Remote Patient Monitoring and Chronic Care Management provide a patient-centered solution that enhances adherence to medication and lifestyle modifications, ultimately leading to improved health outcomes. Empowering patients to take ownership of their health journey is at the heart of successful care management, ultimately paving the way for more successful and sustainable results for their doctor.
Utilizing tools such as remote monitoring and care navigation can help healthcare providers gather patient-generated health data, tailor interventions to patients’ needs, and promote patient engagement. By empowering patients with the knowledge and confidence to take control of their health, they become active participants in their care journey, resulting in improved adherence to treatment plans and enhanced overall well-being.
Remote Patient Monitoring can also help reduce healthcare costs, eliminating the need for in-person visits and reducing hospital readmissions. By leveraging technology and personalized support from care navigators, patients can access the resources and guidance they need to achieve lasting weight loss success and improved health outcomes.
Conclusion: How Health Care Professionals Can Promote Healthy Weight Loss for Obese Patients
Remote monitoring and care management services are powerful tools for managing obesity among patients using newer drug therapies in combination with lifestyle modifications. These medications can promote weight loss, but long-term success depends on continuous monitoring and support.
Virtual care management programs, such as Remote Patient Monitoring, provide healthcare providers with real-time data, allowing them to adjust medication dosages and customize interventions based on individual patient needs. Additionally, remote care management programs empower patients through remote consultation and education, enhancing their adherence to both medication regimens and lifestyle modifications.
By emphasizing a comprehensive care plan and adopting a patient-centered approach, remote care management not only improves health outcomes but also reduces healthcare costs. Through the integration of these strategies, healthcare providers and patients can work together to achieve sustainable weight loss and improved overall well-being.
At HealthSnap, our care navigators are expertly trained to cultivate patient self-efficacy and health literacy, which are essential for realizing care plan goals and boosting patient outcomes. We prioritize understanding each patient’s unique needs and readiness for change. By offering personalized support tailored to individual circumstances with the incorporation of family members and caregivers, we ensure an empathetic and customized approach to weight management as a standalone option for obesity management or as a complementary solution to a patient’s current obesity management treatment plan.
Takeaways:
-
Healthcare providers can utilize Remote Patient Monitoring to adjust medication dosages and tailor interventions to patients’ needs, helping adults achieve successful weight loss.
-
Care navigation supports patient-centered solutions, enhancing adherence to medications, can treat symptoms occurring, and supporting lifestyle modifications that lead to improved health outcomes.
-
Remote care management empowers each patient and family with knowledge and confidence to take control of their health journey, resulting in better adherence to treatment plans and overall well-being.
-
Leveraging technology and RPM data also reduces healthcare costs by eliminating the need for in-person visits with a doctor as well as reducing hospital readmissions.
-
Ideally, care navigators should be trained to cultivate patient self-efficacy and health literacy toward realizing long-term weight loss success through personalized support and tips tailored to individual circumstances.

HealthSnap: The Best Remote Monitoring and Chronic Care Management Company for Obesity Management
The growing role of Remote Patient Monitoring (RPM) and Chronic Care Management (CCM) software companies represents a significant shift toward patient-centered, comprehensive care for individuals with chronic conditions.
One of the key metrics to assess the capability and performance of a virtual care management company, HealthSnap comes out on top among various leading digital health service providers.
Over the last seven years, HealthSnap has emerged as an industry leader in Chronic Care Management (CCM) and Remote Patient Monitoring (RPM) technology and services. HealthSnap is more than just an integrated virtual care platform– we’re a proven solution to bring a higher quality of life to people with chronic conditions and their care teams.
Let’s discuss how our all-in-one integrated Virtual Care Platform can help drive your virtual chronic condition management programs. Call today at 888-780-1872 or click here to schedule a demo.










